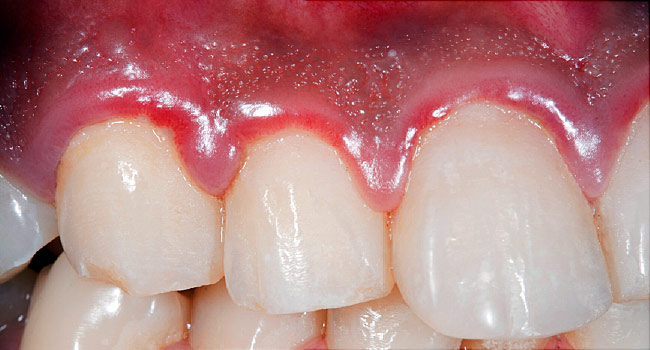
Periodontitis is one of the most common inflammatory disorders, affecting approximately half of adults worldwide. Its link with systemic conditions such as heart disease or diabetes is well-known.
Less well-known is that generalised inflammation is also a potent risk factor for mental health conditions such as depression and anxiety; and conversely, that the likelihood and severity of gum disease can be affected by mental health status.
Periodontal disease links
Increasing evidence suggests that periodontal disease-related inflammation can also be linked to rheumatoid arthritis, some cancers, premature birth and dementia. Whilst the link between mental illness and poor dental health has been long established, it has usually been understood as resulting from the poor self-care and lifestyle often observed in those with poor mental health.
Typically the finger has been pointed at factors such as negligent oral health care, poor diet, smoking and alcohol use. Stress can also reduce saliva volume and affect its composition, which can also contribute to poorer dental health.
In the other direction, any causal effect of poor oral health on mental health has been presumed to be psychological, namely that dental problems can lead to self-consciousness or negative ruminations on health or mortality, which in turn affect psychosocial functioning and mood. However, recent research shows that chronic systemic inflammation directly affects neural systems and behaviour in very specific ways, which suggests that the dental/mental health link is likely to be physiological as well as psychosocial. Increased peripheral cytokines directly affect the brain systems that are known to be involved in depression (such as the hypothalamus, hippocampus and prefrontal cortex), and reduces levels of serotonin, dopamine and norepinephrine in the brain, changes often correlated with mental illness.
Furthermore, inflammation reduces the production of brain-derived neurotrophic factor BDNF, which is central to the creation of new neurons and synaptic connections. Experimentally, the administration of inflammatory agents leads directly to ‘depressive behaviour’ such as social withdrawal, reduced motivation and motor activity, and increased anxiety. Such behaviour is also correlated with natural levels of inflammatory markers in human individuals.
A short-term ‘sickness behaviour’ in response to inflammation that tends to make us lay low and conserve energy when we are injured or fighting an infection makes sense from an evolutionary point of view. However, it is easy to see how chronic inflammation could underpin mental health disturbances if it causes long-term effects on systems that signal reward, mediate threat and responses to it, or affect motivation.
It is important to note that not all people with clinical levels of depression show high inflammation, and conversely, that not all people with inflammation are depressed. Thus systemic inflammation should be seen as one trigger for depression, amongst others.
A resilient person who has few other risk factors for depression may cope with the additional ‘load’ of systemic inflammation without succumbing to depression, whereas someone with several other psychological or inflammatory risk factors may not.